

Les frontières poreuses de la santé : quand humains, animaux et microbes cohabitent
par WILLIAM BISSOU
le 13 novembre 2025
Êtes-vous intéressés par une exploration des limites de la santé humaine à l’ère des zoonoses, du vivant partagé et des vulnérabilités systémiques? De la clinique au territoire, suivez l’itinéraire d'une santé relationnelle.

Il y’a quelques jours, une discussion entre camarades sur la définition de la santé vue sous l’angle du moustique femelle a suscité une curiosité en moi. Et si la santé ne se mesurait pas seulement en signes cliniques, mais aussi en liens. Liens entre humains, entre espèces et entre milieux. S’inspirant du cours sur les approches écosystémiques de la santé, ce bloggue nous invite à penser la santé comme un processus co-construit, situé à l’intersection du social, de l’écologique et du politique.
En parcourant ces pages, on passera du cabinet médical au marais menacé, des indicateurs de morbidité à ceux de biodiversité, des décisions institutionnelles aux voix communautaires.
On y interrogera :
- Comment la santé se vit et se pense en relation avec les écosystèmes ?
- Quelles tensions et injustices émergent lorsque le vivant est fragmenté, surexploité, ou ignoré ?
- Et surtout, comment repenser la pratique, la recherche et l’action collective pour construire des territoires plus sains, plus justes, et plus vivables ?
Bienvenue dans un espace de réflexion critique, d’observation sensible et d'engagement éthique pour une santé qui dépasse les murs de la clinique.
Une santé à l’épreuve des liens
Pendant longtemps, le modèle biomédical classique a pensé la maladie comme une anomalie biologique localisée, la santé comme une affaire de corps individuel : un organisme en équilibre, un patient isolé, une pathologie à guérir. Cette vision héritée de la clinique moderne, a largement structuré les systèmes de santé contemporains. Cependant, avec les crises sanitaires globales telles que le VIH, le SRAS, Ebola, et plus récemment la pandémie de COVID-19, un constat s’impose : la santé humaine n’est pas autonome. Elle est entrelacée avec celle des animaux, des écosystèmes, des infrastructures, des modèles économiques et des imaginaires collectifs. Elle est vulnérable aux effets en cascade d’un monde interconnecté.
C’est ici qu’intervient la perspective écosystémique de la santé, ou écosanté, qui nous invite à sortir de la clinique et à penser les frontières poreuses du vivant.
Le saut d’espèce n’est pas un accident
Selon l’Organisation mondiale de la Santé (OMS) les futures pandémies humaines risquent d’être d’origine zoonotique et que les espèces sauvages en seront la principale source[1]. Les maladies dites zoonotiques[2] représentent aujourd’hui plus de 60 % des maladies infectieuses émergentes. Toutefois, leur émergence n’a rien de naturel. Elle est souvent accélérée ou provoquée par les pratiques humaines telles que la déforestation massive qui pousse les animaux sauvages à côtoyer les humains, les marchés d’animaux vivants, souvent dans des conditions insalubres, l’élevages industriel intensif etc. Ainsi, ce que nous appelons le « saut d’espèce » n’est pas une anomalie biologique, c’est le symptôme d’un modèle de développement destructeur, qui fracture les écosystèmes et multiplie les points de contact à haut risque. Dans cette optique, il semble logique que soigner une épidémie sans traiter ses causes écologiques revient à stériliser une plaie sans retirer l’écharde.
Microbes, alliés et menaces : vers une écologie du minuscule
Souvent perçus comme les ennemis invisibles des humains, les microbes sont pourtant dans la majorité nos alliés. En effet, ils participent à notre digestion, régulent notre immunité, protègent notre peau et même notre cerveau. Le microbiote humain, cet écosystème intérieur de milliards de bactéries et champignons, est façonné dès la naissance : par le type d’accouchement, l’allaitement, le contact avec la nature, la diversité alimentaire. Celui-ci est façonné et modifié en fonction notre mode de vie.
Avec l’urbanisation, la médicalisation excessive (antibiotiques), l’alimentation industrielle et la déconnexion avec le vivant, cette richesse microbienne se fragilise avec pour conséquence une croissance des maladies inflammatoires, auto-immunes et allergiques.
Protéger notre microbiote ne relève pas seulement de la médecine, cela exige une écologie du soin[3], où l’humain, ses microbes et son environnement forment un continuum fragile qui protège également notre santé mentale.
Santé mentale et territoire : l’invisible connexion
L’autre champ de la santé longtemps resté marginal notamment dans les pays du sud global est la santé mentale. Bien que mieux reconnue aujourd’hui, ses liens profonds avec l’environnement restent peu étudiés. Pourtant, les recherches montrent que le contact régulier avec des espaces naturels améliore la concentration, diminue le stress, réduit les symptômes anxieux et dépressifs[4]. À l’inverse, vivre dans des environnements bruyants, pollués, sans accès à la nature, augmente la charge mentale, l’irritabilité, les troubles du sommeil[5]. D’autres études ont montré que la perte ou la transformation brutale de son territoire cause chez les humains la solastalgie, tandis que catastrophes climatiques passées, présentes et futures sont responsables de « l’éco anxiété » ces troubles de la santé nous rappellent que notre équilibre psychique est enraciné dans un lieu. Quand ce lieu est détruit à cause de la déforestation, l’extraction minière, le déplacement forcé, la santé mentale s’effondre avec.
Inégalités écologiques, inégalités sanitaires
La crise climatique et écologique ne touche pas tout le monde de la même manière. Elle renforce des inégalités sociales et territoriales préexistantes. Cela suppose que « les populations pauvres vivent souvent dans les zones les plus polluées, inondables ou exposées aux risques climatiques, que les femmes, dans de nombreux contextes, sont plus exposées aux risques environnementaux à cause de leur rôle dans la gestion de l’eau, de la nourriture, ou de la santé des enfants, et que les peuples autochtones voient leur santé menacée par la perte de biodiversité, la contamination des sols et des eaux, et l’accaparement de leurs terres ».[6] Réfléchir à la santé, c’est donc penser aussi la justice sociale et environnementale. Car il n’y a pas de santé durable sans équité.
Vers une santé relationnelle
Face à ces constats, que faire ? Il ne s’agit pas seulement d’élargir la définition de la santé, mais de changer notre manière de penser le soin. De passer de la réparation à la prévention, de l’individu au collectif, du symptôme à l’écosystème, ou encore de la séparation au vivre-ensemble du vivant. Les approches écosystémiques nous proposent une santé relationnelle, dans laquelle soigner un humain, c’est aussi préserver son environnement, protéger un territoire, c’est préserver des liens culturels, affectifs, biologiques et dialoguer entre disciplines, savoirs et acteurs devient une nécessité éthique et stratégique.
[1] https://fr.worldanimalprotection.ca/blogs/comprendre-les-zoonoses/
[2] Les maladies zoonotiques (zoonoses) sont des maladies ou des infections transmissibles des animaux aux êtres humains
[3] Truc, H. et Alderson, M. (2010). Mieux comprendre l'écologie humaine dans le contexte de la pratique des soins infirmiers. Recherche en soins infirmiers, 101(2), 4-16. https://doi.org/10.3917/rsi.101.0004.
[5] https://www.inspq.qc.ca/en/node/32764
[6] Notre Affaire à Tous. (2020). Un climat d’inégalités : Les impacts inégaux du dérèglement climatique en France. https://notreaffaireatous.org/.
Le Tupiniquim




When Beavers Build Better Health: What Nature’s Engineers Teach Us About Healing Ecosystems and Communities
By Shona Thorne
September 15, 2025

Photo by Tim Umphreys on Unsplash
What if one of the best public health workers in your community had a flat tail and sharp teeth?
It sounds like the beginning of a joke—but it’s a serious thought.
In these uncertain times of climate disruption, chronic disease, and social fragmentation, a surprising hero has surfaced: the beaver. More than just a representation of Canadian wilderness, the beaver has become a natural symbol of an idea whose time has come — Ecosystem Approaches to Health, or EcoHealth.
But this isn’t just a story about how amazing beavers are. It’s a story about how nature-based solutions can simultaneously support environmental, physical, and mental health—and why ignoring these connections puts all of us at risk.
What Is EcoHealth, Anyway?
EcoHealth is more than a catchy term. It’s a transdisciplinary approach that recognizes how human health is intrinsically tied to the health of our ecosystems. It invites us to look beyond doctors’ offices, clinics and hospitals, and instead to consider forests, farms, watersheds, and wetlands as part of our health infrastructure.
Beavers embody this idea perfectly. These ecological engineers reshape landscapes by building dams that create wetlands. In turn, wetlands filter waterbodies, help recharge aquifers, buffer against floods and fires, and boost biodiversity. But that’s not all. The benefits ripple out to human health too.
Beaver-built wetlands help:
- Cool local microclimates, offering natural protection from heatwaves
- Support food chains, including fish and edible plant life
- Create calming environments shown to improve mental well-being
A growing body of research confirms what many already feel: spending time in nature reduces stress, lowers blood pressure, and improves mood. Spending time in biodiverse natural environments doesn’t just soothe the mind—it helps shape the body’s microbiome, influences immune resilience, and reminds us that we are, quite literally, ecosystems ourselves.
A major 2020 international study from the University of Exeter found that ‘blue spaces’—lakes, rivers, and wetlands—are just as beneficial for mental health as green spaces and that encouraging more blue space experiences during childhood, whether it’s playing by creeks or shores, exploring wetlands, could be a simple yet powerful way to support the mental well-being of future generations.
In this way, beavers are quietly beavering away to keep offering ecosystem gifts that nourish both planetary and personal well-being.
Beaver Comebacks, Health Comebacks: A BC Case Study
Centuries of beaver trapping for fur devastated wetland ecosystems but the tide is turning. In early 2023, the B.C. Wildlife Federation (BCWF) launched the 10,000 Wetlands initiative, aiming to restore and enhance wetland systems across the province.
A central part of this effort involves installing Beaver Dam Analogues (BDAs)—structures that mimic natural beaver dams - to stimulate ecosystem restoration and biodiversity. But this isn’t just about science; it’s also about reconciliation. The BCWF is working with First Nations and Indigenous communities to ground these projects in traditional knowledge systems—ones that have long recognized the inseparability of land, health, and spirit.
The goals of this initiative are many:
- Slow down water loss
- Mitigate drought
- Restore salmon habitat
- Rebuild cultural connections to the land
And the outcomes?
- Improved food security through healthier aquatic ecosystems
- Reduced wildfire risk, as wetlands act as natural firebreaks
- Improved mental wellness and youth engagement, as communities reconnect with land stewardship
This is EcoHealth in action: seeing nature not as a backdrop, but as a co-therapist, co-teacher, and co-guardian of community well-being.
Now What? From Beavers to Better Policy
What does this mean for health professionals, educators, and policymakers?
First, we must broaden our definition of health infrastructure. Wetlands, forests, rivers—and yes, beavers—aren’t just ecological luxuries. They are vital components of our shared health system.
Second, we need to invest intentions and time in building transdisciplinary relationships. That means bringing ecologists, doctors, Indigenous elders, urban planners, and youth together to co-create solutions. The beaver may not attend policy summits, but it models the power of natural restoration better than most human interventions.
Third, we need to shift from siloed to systems thinking. EcoHealth is not about isolating sectors. It’s about recognizing the full web of life and well-being, and learning how to thrive within it.
Call to Action
Start small. Work together. Build connections.
- If you're a health professional, explore how natural spaces can become part of your prescriptions.
- If you're a policymaker or planner, integrate wetland restoration into your public health and climate adaptation strategies.
- If you're an educator, take students of every age outside—and into deeper conversations about land-based knowledge.
- And if you’re a citizen, champion nature as a health ally in your neighbourhood, town, or territory.

Beavers don’t just build dams.
They build resilience, and above all they don’t quit.
In a world stumbling between ecological collapse and hopeful regeneration, resilience and perseverance might be some of the most powerful medicine we’ve got.
Photo by Ng Sze En on Unsplash
|
“Beavers, the animal that doubles as an ecosystem, are ecological and hydrological Swiss Army knives, capable, in the right circumstances, of tackling just about any landscape-scale problem you might confront. Trying to mitigate floods or improve water quality? There’s a beaver for that. Hoping to capture more water for agriculture in the face of climate change? Add a beaver. Concerned about sedimentation, salmon populations, wildfire? Take two families of beaver and check back in a year. If that all sounds hyperbolic to you, well, I’m going to spend this book trying to change your mind.” ― Ben Goldfarb, Eager: The Surprising, Secret Life of Beavers and Why They Matter |
Die Another Way: Finding sustainability and reciprocity in death
By Rachael Young
September 15, 2025
 With a scalpel in hand, I inspected the palm in front of me closely. Stealing a glance to my textbook, I took a deep breath and began to cut. Methodically, I parsed apart layers of skin and fascia, eyes always seeking the intricate network of muscles, tendons and nerves that lay just below. Tracing around delicate wrinkles, I advanced slowly toward the fingertips. Despite the shakiness of my unpracticed hand, it was peaceful, and my mind began to wander. This was not the first time I’d dissected in the cadaver lab, but at just a few weeks into my intro anatomy course, I was still uncertain. Uncertain about what tools to use, uncertain about how to find the tiny nerves that would appear on my exam, and above all, uncertain about how to feel.
With a scalpel in hand, I inspected the palm in front of me closely. Stealing a glance to my textbook, I took a deep breath and began to cut. Methodically, I parsed apart layers of skin and fascia, eyes always seeking the intricate network of muscles, tendons and nerves that lay just below. Tracing around delicate wrinkles, I advanced slowly toward the fingertips. Despite the shakiness of my unpracticed hand, it was peaceful, and my mind began to wander. This was not the first time I’d dissected in the cadaver lab, but at just a few weeks into my intro anatomy course, I was still uncertain. Uncertain about what tools to use, uncertain about how to find the tiny nerves that would appear on my exam, and above all, uncertain about how to feel.
I had a strange relationship with the body in front of me. In some ways, I knew this person more intimately than anyone had known them in life. I had literally seen the depths of their heart, but I didn’t know their name. I was the last person to ever hold their hand. Who was the first, I wondered. Had this hand played an instrument, worn a wedding ring, cradled a child? I will never know. The only thing I am sure of, is that this person’s final act in life was to give themselves completely to others in death. It was comforting to witness death as a gift like this. I felt less uncertain, and more grateful.
My focus eventually returned to the dissection. By the end of lab, I’d revealed much of the palmar surface; I could name and identify every muscle, artery, tendon, nerve, and bone that was tested on the midterm. I’ve since forgotten much of this anatomy, but I remember the feeling of holding that hand. I remember the way it held mine back. I remember the space it gave me to reflect on the impact of our bodies after we die.
Outside of these rather one-sided conversations in cadaver labs, I find that good discussions about death can be hard to come by. In the rare cases when we are encouraged to talk about death, the focus is often on practicalities or the psychological benefits of doing so. While I recognize the importance of these approaches, there is a more pressing issue that should motivate us to prioritize this dialogue; our death rituals are harming ecosystems globally1. Over 300,000 people die every year in Canada2, the vast majority are either cremated, or embalmed and buried3. Both of these practices exacerbate existing threats to human and more than human life1.
Cremation is the most common death practice in Canada3, and it is a source of several concerning emissions4,5. In the cremation process, carbon dioxide is released from the natural gases burned to power furnaces as well as from the organic carbon stored in human bodies1. This contributes to the global greenhouse gas effect and ongoing climate crisis, but there are further hazards still. Compounds that accumulate in the human body such as heavy metals like mercury, volatile organic compounds like benzene, and other concerning chemicals, are routinely emitted during cremation5. A study in British Colombia, for example, found that crematoriums accounted for over 7% of atmospheric mercury emissions in the province6. Once released, these pollutants may enter any part of the ecosystem and endanger the health of many living things5.
Like cremation, traditional embalming and burial practices produce a number of harmful environmental impacts1. After burial, heavy metals, pathogens, and hazardous chemicals from embalming, like formaldehyde, leach from bodies into the surrounding soil7–9. Eventually, these pollutants enter ground water systems, and spread throughout the ecosystem7,9. Then, there are the materials involved in the process. From coffins to grave markers, resources are extracted and may be transported long distances to complete the burial process1. There are also land-use concerns. Cemeteries can take up large areas, which may contribute to habitat fragmentation and other ecological concerns10. Grass lawns are common and require large amounts of water while contributing little to biodiversity1,10. Together, these factors have concerning implications for the health and well-being for humans, animals and plants alike.
In recent years, green burial practices have emerged as a potential solution to these challenges1,10. While there are promising options like water cremations that reduce harmful emissions, natural burials, and traditional Indigenous practices, there remain significant challenges1,10. These alternatives are often expensive, inaccessible, or not legally recognized under colonial systems10. Complex social, cultural, and religious practices may also impact choices around death1. So how do we make sustainable, lasting changes? Beyond small steps like opting for alternative cremation, avoiding embalming and choosing local, natural materials for grave markers, I don’t think there is a simple answer. I do, however believe that talking more openly about death and the impacts of death practices on ecosystems is a good place to start.
Conversations about death can be hard, but I often find them easier when I think back to my experiences in the human anatomy lab at the University of Guelph. It’s difficult to articulate what a privilege it was to learn from the body donors. I can confidently say that over the two years I spent in the anatomy program, they taught me far more than just the structure and function of the human body. I cannot thank someone who is dead, so instead I find myself asking how I can give to others like they gave to me; I invite you to do the same. How can we make our deaths and death practices more sustainable? How can we become more like the hand that held mine when I was so uncertain? How can we turn death into a gift for all living things?
References
1. Nosi, C., D’Agostino, A., Ceccotti, F. & Sfodera, F. Green funerals: Technological innovations and societal shifts toward sustainable death care practices. Technol Forecast Soc Change 207, 123644 (2024).
2. Deaths, by month. https://www150.statcan.gc.ca/t1/tbl1/en/tv.action?pid=1310070801.
3. Industry Statistical Information - Cremation Association of North America (CANA). https://www.cremationassociation.org/industrystatistics.html.
4. Xue, Y. et al. Emission characteristics of harmful air pollutants from cremators in Beijing, China. PLoS One 13, e0194226 (2018).
5. Mari, M. & Domingo, J. L. Toxic emissions from crematories: A review. Environ Int 36, 131–137 (2010).
6. Piagno, H. & Afshari, R. Mercury from crematoriums: human health risk assessment and estimate of total emissions in British Columbia. Can J Public Health 111, 1011 (2020).
7. Zychowski, J. Impact of cemeteries on groundwater chemistry: A review. Catena (Amst) 93, 29–37 (2012).
8. Ezenwa, I. M. et al. Burial leakage: A human accustomed groundwater contaminant sources and health hazards study near cemeteries in Benin City, Nigeria. PLoS One 18, e0292008 (2023).
9. Zychowski, J. & Bryndal, T. Impact of cemeteries on groundwater contamination by bacteria and viruses – a review. J Water Health 13, 285–301 (2015).
10. Green end-of-life options - David Suzuki Foundation. https://davidsuzuki.org/living-green/green-end-of-life-options/.
Nature’s Cure for a Disconnected World
By Megan Tomlison
September 15, 2025
 Nestled within the woodlands of a semi-urban town along the Pacific Coast of British Columbia, a towering Douglas Fir stands like a sentinel —ancient, steady, and quietly dignified. I call her ‘Big Mama.’ For many years, my routine has been to visit this majestic giant at the end of a stressful nursing shift. My practice is to take pause in Big Mama’s presence and lean into her quiet, unconditional support. Without words, she soothes my nervous system and rekindles my spirit. Needless to say, I was heart broken during a recent visit when I found Big Mama defaced by spray paint. The vandalism was sloppy, somewhat illegible and appeared to convey a disturbing message of racial intolerance. A week later, while exploring another nearby forest, I came across three more trees tagged with similar messages.
Nestled within the woodlands of a semi-urban town along the Pacific Coast of British Columbia, a towering Douglas Fir stands like a sentinel —ancient, steady, and quietly dignified. I call her ‘Big Mama.’ For many years, my routine has been to visit this majestic giant at the end of a stressful nursing shift. My practice is to take pause in Big Mama’s presence and lean into her quiet, unconditional support. Without words, she soothes my nervous system and rekindles my spirit. Needless to say, I was heart broken during a recent visit when I found Big Mama defaced by spray paint. The vandalism was sloppy, somewhat illegible and appeared to convey a disturbing message of racial intolerance. A week later, while exploring another nearby forest, I came across three more trees tagged with similar messages.
It goes without saying that trees are a life-giving organism. They provide shelter, oxygen, and habitat for wildlife. Trees improve soil and water conservation and are a vital solution in mitigating climate change by sequestering carbon dioxide from the atmosphere. The traditional knowledge of Indigenous peoples highlights the significance of trees – in addition to serving as a source of sustenance and medicine, trees are sacred beings deserving of reverent stewardship for the well-being of the eco-systems and its future generations.
Western science is only just beginning to understand the human health benefits associated with trees and the natural world. Phytoncides - antimicrobial organic compounds emitted by trees and plants, similar to essential oils – are thought to mediate health promoting effects and can improve human immune function. Immersing oneself in nature, a therapeutic practice known in Japan as Shinrin-yoku, or forest bathing, appears to benefit human health in a multitude of ways. Increasing research indicates that forms of nature therapy, whereby a meaningful connection to the natural world is established, has been shown to reduce stress, enhance joy and contributes to better sleep. Individuals should seek clinical guidance from a health care provider, however nature therapy may serve as a low risk, complimentary treatment for chronic disease management and improved cognitive function. Youth living with attention deficit hyperactivity disorder (ADHD) may also benefit from just twenty minutes per day of nature therapy as a safe, inexpensive intervention to improve concentration.
The promotion of nature therapy as a legitimate health intervention is gaining momentum, as seen in the BC Parks Foundation PaRx program, whereby regulated health care practitioners prescribe nature therapy to improve overall well-being. That said, access to nature is not evenly distributed, particularly in the context of socio-economic disparity. It is in our collective interest to prioritize access to green spaces for human health and for the protection of the natural world. It is broadly accepted that the more time people spend in nature, the more likely they are to protect it. Initiatives such as PaRx may therefore serve as a dual strategy: improving human health and fostering ecosystem stewardship.
The protection of forests and wild spaces requires a multifaceted approach. While individual actions and grassroots initiatives are vital, all levels of government share responsibility for environmental protection – particularly as colonial driven agendas of extraction persist. Governments must work diligently to ensure Indigenous voices and traditional knowledge are central to decisions regarding natural resource management. With growing pressure to densify urban spaces, municipal leaders must prioritize access to green spaces for all residents as a critical measure for public health.
The graffiti on Big Mama’s bark wasn’t just vandalism—it was a symptom of a deeper disconnection, a warning sign of how far we’ve strayed from our relationship with the natural world. But disconnection can be healed. Each walk in the woods, each breath among trees, each moment of quiet wonder is a step back toward wholeness.
Trees don’t just hold up the sky—they hold up our future. It’s time we hold them up, too.
We are what we eat – Healing through local food systems
By Fenja Neumann
August 28, 2024

Local market garden in Mecklenburg Western Pommerania, Germany. © Fenja Neumann
Have you ever heard of the saying “You are what you eat”? Well, we literally are. Modern research has proven that the gut is directly connected to the brain, which means that the food we eat influences our brain chemistry1. Not only can food determine our mood, but it also affects our immune system. Thus, besides providing us with energy and nutrients, food can reduce or enhance diseases and it impacts our biochemistry2. There is a growing awareness that what we put into our mouths is important, but how well do we really eat?
If we take a closer look at the global food system, we will find that it doesn’t nourish us as it should, but rather creates a cascade of health-related problems. As we walk through our supermarkets, it becomes evident that unprocessed food, such as organic vegetables, fruits, grains, legumes, and raw animal products, is much more expensive than processed goods. One reason for this is that our globalised food system heavily relies on imports3. In 2022, approximately 75% of vegetables and 37% of fruit were imported, largely from the US20,21. However, in 2019, Canada also exported around 1 million tonnes of vegetables, while over 2 million tonnes were still imported21. This indicates that greater self-sufficiency is possible if Canadian produce largely remains within the domestic food system. Quebec, for example, improved its self-sufficiency for greenhouse-grown vegetables from 30% to 50%, now targeting 80%22.
One aspect that surprised me is that five large retailers hold 76% of the market share in Canada23. And while the net revenues of Canadian grocers have been steadily growing (e.g., from 1.4 billion in 2017 to 2.6 billion $ in 20214), the prices for the consumer are skyrocketing, with an increase of over 10% for most provinces in 2022 alone5. With 6.9 million (17.8%) food-insecure Canadians in 20236, it seems outrageous that approximately 20% of all food produced in the country is wasted every year19.
Sadly, the food that is affordable for lower-income households is often highly processed, nutrient-deficient, and detrimental to our health7. This kind of diet is frequently associated with heart disease, diabetes, cancer and strokes. Moreover, the global food system is built on a highly unsustainable industrial agriculture. It enhances climate change, degrades our soils, pollutes our waters and poisons our nature. And as we are an integral part of nature, it directly affects us. It has been proven, for example, that certain pesticides can promote cancer, developmental- and reproductive impairments, and changes in the immune system. Unfortunately, industrial meat production looks just as dire. Factory farming is not only an ethical disaster, it also increases the spread of zoonotic diseases between animals and humans and promotes antimicrobial resistance, both of which can be fatal7. I think it’s safe to say that if the price of food is health, it’s too high.

Crop field being sprayed with pesticides. © PublicDomainPictures from Pixabay
But where do we start to heal from a system that literally makes us sick? The answer is quite simple: Locally. The current agricultural industry is very centralised8 – A small number of large-scale farms sell to a few big wholesalers or retailers. While the last pandemic clearly demonstrated that this import-dependent system threatens our food security9, local food systems (LFS) are regarded as more resilient and thus received increasing attention10. They can be interpreted as “collaborative networks that integrate sustainable food production, processing, distribution, consumption, and waste management in order to enhance the environmental, economic, and social health of a particular place”11. The government of Canada considers food as local when it’s produced within the province or 50 km beyond12, whereas it’s only a radius of 20 – 100 km within European countries13. There are many ways to acquire local products, for example at farmers' markets, or directly from the producers. Other options include food boxes, community gardens, community-supported agriculture, food hubs, restaurants, (local) retail, or even wholesale10. But the closer, the better.

Community-supported agriculture (CSA) in Mecklenburg-Western Pomerania, Germany. They farm bio-intensive and regenerative on 1,4 acres and supply 80 households with fresh vegetables once per week. © Fenja Neumann
Local food systems have tremendous benefits on different levels. They support local economies and small-scale, family-owned farms14. While currently, large corporations have the power over our food, LFS can increase our food sovereignty, as they allow us to build relationships with producers and support them in their practices – actively or passively. Being involved in farming can be healing in itself. Reconnecting with nature through gardening bears great potential to improve our mental health15. Small-scale local farms don’t rely on pesticides and antibiotics, as diseases are not spread as easily as in factory farming. While they may still apply it, it’s likely to a much lesser extent, and studies show that local producers often farm organically16. So locally grown food is not only healthier, it also contains more flavour and vitamins due to the short transport routes. This also benefits the climate by saving greenhouse gas emissions. Local farms often have a greater interest in caring for the land they depend on. Sustainable practices help to reduce environmental pollution, biodiversity loss, and soil degradation.
Despite the advantages of LFS, they only account for a small portion of the overall food consumption in Canada. While local in-season vegetables and fruit can be cheaper than in grocery stores17, consumers are unquestionably facing access barriers for some products, especially pricing18. Competing with global players is challenging, and there are still many other economic and political barriers to expanding LFS. Nevertheless, our health depends on the transformation towards sustainable food production, and local food systems are a good starting point. Depending on financial and personal resources, there are many ways to get involved in LFS, for example by:
♥ checking out https://farmfolkcityfolk.ca/ and https://youngagrarians.org/ for local farms, CSA’s and young farmer’s initiatives
♥ growing food in our own yard or community gardens, urban farms, etc.
♥ shopping at farmer’s markets or buying directly from local farmers and producers
♥ getting involved in CSA’s or subscribing to local food boxes
♥ purchasing seasonal and local products in the grocery store
_______
1 Basharat, I. (2023, March 22). You are what you eat: The gut-brain connection. Retrieved from https://oxsci.org/gut-brain-connection/
2 Mierziak, J., Kostyn, K., Boba, A., Czemplik, M., Kulma, A., & Wojtasik, W. (2021). Influence of the bioactive diet components on the gene expression regulation. Nutrients, 13(11), 3673. https://doi.org/10.3390/nu13113673
3 Canada, A. a. A. (2020, May 27). Canada’s food security dependencies. Retrieved from https://agriculture.canada.ca/en/sector/data-reports/canadas-food-security-dependencies
4 Government of Canada. (2019, March 1). Grocery stores - 4451 - Retail revenues and expenses - Canadian Industry Statistics - Innovation, Science and Economic Development Canada. Retrieved from https://ised-isde.canada.ca/app/ixb/cis/retail-detail/4451
5 Charlebois, S., Rankin, A., Taylor, S., Keselj, V., Abebe, G., Colombo, S., . . . Humes, K. (2023). Canada’s Food Price Report 2023. (J. Lord, Ed.). Retrieved from https://cdn.dal.ca/content/dam/dalhousie/pdf/sites/agri-food/Canada%27s%20Food%20Price%20Report%202023_Digital.pdf
6 PROOF - Food Insecurity Policy Research. (2024, April 26). How many Canadians are affected by household food insecurity? - PROOF. Retrieved from https://proof.utoronto.ca/food-insecurity/how-many-canadians-are-affected-by-household-food-insecurity/
7 United Nations Environment Programme. (n.d.). 9 ways food systems are failing humanity. Retrieved from https://www.unep.org/news-and-stories/story/9-ways-food-systems-are-failing-humanity
8 Thu, K. (2009). The centralization of food systems and political power. Culture & Agriculture, 31(1), 13–18. https://doi.org/10.1111/j.1556-486x.2009.01013.x
9 BC Centre for Disease Control. (2024). EXAMINING THE CONSEQUENCES OF THE COVID-19 PANDEMIC: Food insecurity situation. Retrieved from http://www.bccdc.ca/Health-Professionals-Site/Documents/societal_consequences/Food_Insecurity.pdf
10 Enthoven, L., & Van Den Broeck, G. (2021). Local food systems: Reviewing two decades of research. Agricultural Systems, 193, 103226. https://doi.org/10.1016/j.agsy.2021.103226
11 Feenstra, G., & Campbell, D. C. (2013). Local and regional food systems. In Springer eBooks (pp. 1–9). https://doi.org/10.1007/978-94-007-6167-4_73-1
12 Statistics Canada. (2023, September 5). The Daily — Survey on Local Food and Beneficial Management Practices, 2022. Retrieved from https://www150.statcan.gc.ca/n1/daily-quotidien/230905/dq230905a-eng.htm
13 European Commission. (2013). Short Food Supply Chains and Local Food Systems in the EU. A State of Play of their Socio-Economic Characteristics (report EUR 25911 EN). https://doi.org/10.2791/88784
14 Michigan State University - MSU Extension. (2019, January 17). Seven benefits of local food. Retrieved from https://www.canr.msu.edu/news/seven-benefits-of-local-food
15 Thompson, R. (2018). Gardening for health: a regular dose of gardening. Clinical Medicine, 18(3), 201–205. https://doi.org/10.7861/clinmedicine.18-3-201
16 Link, A., & Ling, C. (2001, February 7). Farmers’ markets and local food systems. Retrieved from https://www.crcresearch.org/crc-case-studies/farmers-markets-and-local-food-systems
17 Pirog, R., & McCann, N. (2009). Is local food more expensive? A Consumer Price Perspective on Local and Non-Local Foods purchased in Iowa. Retrieved from https://www.leopold.iastate.edu/files/pubs-and-papers/2009-12-local-food-more-expensice-consumer-price-perspective-local-and-non-local-foods-purchased-iowa.pdf
18 Carter, R. (2017, January 26). The true cost of local food | UVM Food Feed. Retrieved from https://learn.uvm.edu/foodsystemsblog/2017/01/24/true-cost-of-local-food/
19 Canada, E. a. C. C. (2019, June 28). Taking stock: Reducing food loss and waste in Canada. Retrieved from https://www.canada.ca/en/environment-climate-change/services/managing-reducing-waste/food-loss-waste/taking-stock.html
20 York University. (n.d.). Reliance on exports | Food Policy for Canada. Retrieved June 10, 2024, from https://foodpolicyforcanada.info.yorku.ca/backgrounder/problems/reliance-on-exports/#:~:text=Now%2C%20it%20is%20estimated%20that,US%20(Hui%2C%202022)
21 Agriculture and Agri-Food Canada. (2020, August). Statistical Overview of the Canadian Vegetable Industry. Retrieved from https://publications.gc.ca/collections/collection_2020/aac-aafc/A71-37-2019-eng.pdf
22 Wheeler, M. (2023, January 3). Le Québec est autosuffisant à 50 % pour les fruits et légumes produits en serre. Radio-Canada. Retrieved from https://ici.radio-canada.ca
23 U.S. DEPARTMENT OF AGRICULTURE [USDA]. (2022, July). Retail Foods (CA2022-0018). Retrieved from https://apps.fas.usda.gov/newgainapi/api/Report/DownloadReportByFileName?fileName=Retail%20Foods_Ottawa_Canada_CA2022-0018.pdf
Mother Nature's Lessons in Healing and Forgiveness: Reciprocating Hope for Our Shared Future
By Jaden Gornall
August 28, 2024
On the evening of December 18, 2023, I slipped down a steep embankment in the heart of the Cascade Mountains. Immobilized by injury, temperatures dipped to -8°C as overnight I lay in deep intimacy with my surroundings, held against the quietude of the mountain’s snow-blanketed bosom. By the time my campmate found me the next morning, hypothermia had taken hold, and my left leg was fully paralyzed. I was transported swiftly to Abbotsford Hospital, where my condition escalated to “life over limb.” My left leg was amputated above the knee the next day.
Camping this past May on Cortes Island in the context of the CoPEH-Canada hybrid course has been my first experience doing so with a prosthetic leg, having received this carbon accoutrement 3 weeks prior. A seasoned camper, practical considerations I had never contemplated, like where to plug in my leg to charge at night, became my reality. Keenly observing how nature responds to injury with grace has inspired my healing, igniting my curiosity around a question: What lessons does nature offer about healing that can we translate into our roles and responsibilities in “healing back” eco-social systems?
Even in the face of humanity’s transgressions against the environment, Mother Nature demonstrates qualities of forgiveness. This series of photos explores variations on this theme, as I observed while visiting the Children’s Forest, a parcel of land that community members are securing as trust in perpetuity for the present and future children of Cortes. Within this old homestead, Nature claims broken items, absorbing and integrating them into its forest scape: Moss grows tenderly around frayed rope. An ancient car becomes a habitat, engulfed into cascades of greenery.
We can observe this resilience similarly in the regrowth of forests after devastating fires. These examples remind us that healing is not about returning to a previous state, but rather about accepting the changes that have occurred, and finding new ways to move forward with resilience. I learned quickly that to resist the loss of my leg was to entrap myself in a cycle of suffering. Befriending and incorporating a carbon fibre and titanium limb as my own has become part of my practice of acceptance, liberating me from rolling a Sisyphean rock up a proverbially endless mountain. The moss, gentle breeze, and ambling ants of the forest were no less welcoming and accepting to the carbon-wielding elements of my body than to my flesh when visiting the Children's Forest, so I ask myself, in what ways can I relate to myself with that same flexibility and grace?
Nature’s ability to accommodate a continual onslaught of human-induced climate change is certainly not limitless, however, and our timely action is urgently required. How can what we learn from nature’s demonstrations of healing teach us to promote future positive actions rather than enabling further desecration, through the co-benefits of practicing forgiveness?
Climate change can lead to “psychoterratic” or earth-related mental health issues, such as eco-anxiety, eco-paralysis, solastalgia, and eco-nostalgia, terminology defined by Glenn A. Albrecht.1 Eco-anxiety refers to worry and stress related to the ecological crisis, which is very common among children and youth. Other phenomena include eco-guilt from violating environmental values, eco-grief over loss of environment and identity, and solastalgia–the sorrow felt when one's beloved homeland deteriorates, or “the homesickness you have when you are still at home.”1 Depression, suicidal ideation, and post-traumatic stress disorder are further manifestations of this mental health decline.2
Perhaps the greatest barrier to propelling action is eco-paralysis, the inability to meaningfully respond to ecological challenges, characterized by apathy, complacency, or disengagement stemming from the overwhelming nature of environmental issues.1 This may arguably lead to defense mechanisms such as climate change denial.3
An intergenerational conflict narrative has emerged against the backdrop of climate change discussions, underscoring mental health concerns. Elders are often blamed for committing cavalier and irreversible transgressions against our Planetary Health, consequences that future generations will have to live with as we emerge into what has been termed as the human-dominated anthropocene. Meanwhile, youth are often angry and hopeless at their unconsenting roles within the planetary predicaments they face.
Although anger can at times motivate pro-environmental action, sadness–perhaps an extension of hopelessness–can inhibit it.4 Prolonged feelings of anger and holding grudges may also exacerbate the health burdens of climate destruction, rather than leading to cooperative solutions. In a study that measured the physiological impacts of ruminating on past transgressions and holding grudges, it was found that participants experienced increases in blood pressure, heart rate, sweating, and negative emotions like anger and anxiety.5 However, when participants conversely practiced empathy and imagined forgiving their offenders, their physical arousal and stress reactions decreased to normal waking levels.5 In other words, forgiveness is ostensibly protective to our individual health, and by extension–to Planetary Health.
In Earth Emotions: New Words for a New World, Albrecht examines the range of positive and negative emotions humans experience towards the environment, arguing for the need to cultivate a hopeful vocabulary of positive eco-emotions to reignite our biophilia and transition from the human-centric Anthropocene to a Symbiocene era founded on symbiotic science's revolution in thinking about humanity's relationship with the planet.6 Albrecht contends that by developing this new emotional lexicon, we can extract ourselves from environmental desolation and reaffirm our ancient love of life for our home planet through a dramatic shift grounded in contemporary symbiotic science's material, ethical, political, and spiritual principles.6
It is critical to remember that intergenerational conflicts surrounding climate change are not simply conceptual, executed amongst faceless “others”. These tensions underlie relationships between children, parents, and grandparents, degrading the cohesion of families and communities, the very fabric of mutual support and well-being, which may fortify us to address climate injustices. Meanwhile, on a relational level, forgiveness has numerous benefits, including helping to re-establish more positive, benevolent, and cooperative goals within relationships.7
The Children’s Forest is a thriving example of the co-benefits of intergenerational and symbiotic action towards climate change. As one community elder and leader highlighted, an unanticipated and enduring effect of the Children’s Forest initiative has been the deepening of intergenerational relationships. Biophilia–love of life, and all that is living–by its very nature extends to our relationships with each other, and to loving one another. Nature shows this to us unconditionally, and may we reciprocate its lessons through our human-human and human-environment relationships.
References
1. Albrecht G. Chronic Environmental Change: Emerging “Psychoterratic” Syndromes. International and Cultural Psychology. 2011;43–56.
2. Clayton S, Manning C, Krygsman K, Speiser M. Mental Health and Our Changing Climate: Impacts, Implications, and Guidance [Internet]. 2017 Mar. Available from: https://www.apa.org/news/press/releases/2017/03/mental-health-climate.pdf
3. Maroni E. Do Most Americans Believe in Human-Caused Climate Change? It Depends on How You Ask. [Internet]. The Annenberg Public Policy Center of the University of Pennsylvania. 2019 [cited 2024 May 17]. Available from: https://www.annenbergpublicpolicycenter.org/do-most-americans-believe-human-caused-climate-change/
4. Contreras, A., Blanchard, M. A., Mouguiama-Daouda, C., & Heeren, A. When eco-anger (but not eco-anxiety nor eco-sadness) makes you change! A temporal network approach to the emotional experience of climate change. Journal of anxiety disorders. 2024;102,102822.
5. Worthington EL, Witvliet CVO, Pietrini P, Miller AJ. Forgiveness, Health, and Well-Being: A Review of Evidence for Emotional Versus Decisional Forgiveness, Dispositional Forgivingness, and Reduced Unforgiveness. Journal of Behavioral Medicine. 2007 Apr 24;30(4):291–302.
6. Albrecht G. Earth Emotions: New Words for a New World. Ithaca London Cornell University Press; 2019.
7. Fincham FD. Forgiveness: Integral to a science of close relationships? Prosocial motives, emotions, and behavior: The better angels of our nature. 2010;347–65
Hot Flashes and Heat Waves: The Intersection of Climate Change, Gender, and Menopause
By Mackenzie Bosch
August 28, 2024
ⓒ Tourism Burnaby
Increasingly prevalent across the globe, climate-related events such as rising temperatures, forest fires, droughts, and natural disasters are significantly impacting ecosystem health. These impacts include species endangerment, loss of biodiversity, and severe consequences for human health. A critical but often overlooked aspect is the gendered differences in how climate change affects health, with women facing unique challenges that frequently lead to worse outcomes.
Research on women's health and climate change has predominantly focused on early reproductive and maternal health, leaving out a key demographic—aging women, particularly those undergoing menopause. Menopause, a pivotal phase marking the natural end of a woman's reproductive years, affects various aspects of health and already represents a site of health inequity for middle-aged women and individuals with a uterus. Many women report significant health disparities during menopause, including a lack of awareness about symptoms and treatment options, as well as inadequate care and understanding from healthcare providers.
Celebrate Women's Health Through Japanese Calligraphy Art ⓒ Easy-Peasy.AI
Recent studies indicate that climate and environmental changes can exacerbate menopause symptoms and related health impacts. For instance, rising temperatures can increase the prevalence and severity of hot flashes and night sweats, affecting an estimated 79% of those in menopause. Higher temperatures may also disrupt sleep and negatively impact mental health, leading to increased stress, anxiety, depression, and cognitive issues such as "brain fog." Warmer months are already associated with poorer sleep quality, and extreme temperatures can impair cognitive performance, though further research is needed to confirm this in menopausal individuals.
Environmental pollutants can also impact menopause physiology. Studies indicate that increased exposure to pollutants (e.g., ozone, carbon monoxide), which are on the rise due to climate change, can alter ovary aging and the timing of menopause. For example, prolonged exposure to these pollutants has been associated with an earlier onset of menopause. This is concerning as early menopause is shown to have its own set of health issues, including negative impacts on cognition, mood, cardiovascular health, and a higher risk of early mortality. Additionally, menopausal women who are already vulnerable, face an increased likelihood of bone loss and cognitive decline when exposed to higher pollution levels.

Image courtesy of Fred Murphy under CC BY-ND-NC 1.0. © Pi Media
Addressing these significant health inequities exacerbated by climate change requires a comprehensive response that tackles both the gaps in menopause treatment and the broader impacts of climate change and environmental factors that worsen menopause symptoms and physiology. This entails working towards greater climate action, improving awareness and education about menopause among healthcare professionals and the general population, increasing research on women's health, and integrating climate change and human health considerations throughout the healthcare system.
Promoting social justice, eco-social health equity, and enhancing the quality of life for those experiencing menopause is not just necessary—it's imperative. Advocating for change and fostering collaboration among researchers, healthcare providers, policymakers, and communities is essential to develop innovative solutions that prioritize women's health in the context of our changing environment. It is only through coordinated efforts and decisive action that we can ensure a healthier, more equitable future for all humans and our planet.
Resources:
1. Menopause Foundation of Canada. The Silence and the Stigma: Menopause in Canada [Internet]. Canada: Menopause Foundation of Canada; 2022. Available from https://menopausefoundationcanada.ca/menopause-in-canada-report/
2. Cucinella L, Tiranini L, Nappi RE. Impact of climate and environmental change on the menopause. Maturitas [Internet]. 2023 Dec 1;178:107825. Available from: https://doi.org/10.1016/j.maturitas.2023.107825
3. Smith JN, Van Daalen KR, Venkatraman R. Climate change and its potential impact on menopausal hot flashes: a commentary. Menopause [Internet]. 2020 Feb 24;27(7):816–7. Available from: https://doi.org/10.1097/gme.0000000000001521
4. Faubion SS, Kuhle CL, Shuster LT, Rocca WA. Long-term health consequences of premature or early menopause and considerations for management. Climacteric [Internet]. 2015 Apr 7;18(4):483–91. Available from: https://doi.org/10.3109/13697137.2015.1020484
5. Osman-Elasha B. Women...In the shadow of climate change | United Nations [Internet]. UN Chronicle, United Nations. 2009 [cited 2024 May 31]. Available from: https://www.un.org/en/chronicle/article/womenin-shadow-climate-change
6. McCarthy J. Understanding why climate change impacts women more than men [Internet]. Global Citizen. 2020 [cited 2024 Jun 14]. Available from: https://www.globalcitizen.org/en/content/how-climate-change-affects-women/
Le chant des Îles : La micromobilité pour une biodiversité florissante au Parc Jean-Drapeau
Monica Tanase
le 28 août 2024
Nichées au cœur du fleuve Saint-Laurent, les îles Sainte-Hélène et Notre-Dame forment le Parc Jean-Drapeau, un espace vert majeur au cœur de Montréal. Ici, la nature murmure et les échos des oiseaux rappellent l'importance de préserver ce milieu naturel. Pour renforcer cet écosystème précieux, la micromobilité en libre-service, incluant trottinettes et vélos électriques, émerge comme une solution harmonieuse, promouvant une mobilité douce et respectueuse de l'environnement. Que vous soyez une famille en quête d’aventure ou une personne âgée désirant profiter pleinement de la nature en toute tranquillité, la micromobilité est votre alliée. Explorer plus, aller plus loin.

La micromobilité, une mélodie écologique
La micromobilité rassemble les solutions de déplacement pour de courtes distances, incluant le transport actif (vélo) et d’autres véhicules légers (trottinette électrique) limités à 25km/h (Bretones et Marquet, 2022; Ghaffar et al., 2023). Les vélos à assistance électrique et les trottinettes électriques peuvent être regroupés dans une catégorie plus spécifique de micromobilité électrique qui permet de parcourir les trajets avec moins d’effort physique. La micromobilité en général est une solution flexible, avec des effets positifs sur la santé et un potentiel d'inclusion sociale (Mueller et al., 2015; Bretones et al., 2023; Avila-Palencia et al., 2018; Milakis et al., 2020). De plus, elle peut être très agréable grâce aux expériences kinesthésiques et sensorielles qu'elle procure (Spinney, 2006; Clayton et Musselwhite, 2013).
 |
 |
Ces moyens de transport sont non seulement pratiques, mais aussi respectueux de l'environnement, réduisant la dépendance aux voitures et diminuant ainsi les émissions de gaz à effet de serre. Leur utilisation au Parc Jean-Drapeau aide à diminuer les niveaux de pollution atmosphérique. Moins de voitures signifie moins de dioxyde de carbone et d'autres polluants, ce qui améliore la qualité de l'air et favorise un environnement plus sain pour la flore et la faune du parc.
Réduire la voiture au sein du parc, un choix pour la terre
Actuellement le Parc Jean-Drapeau fait face à une prépondérance de l'utilisation de la voiture sur son territoire. Se déplacer en voiture au sein du parc est comme une fausse note dans une symphonie naturelle. Les impacts négatifs sont nombreux. Les voitures à essence sont responsables de plus de la moitié des émissions mondiales d'oxydes d'azote et d'une proportion significative de particules fines (HEC Montréal Chaire de gestion du secteur de l’énergie, 2023), contribuant ainsi à la pollution de l'air et aux changements climatiques. Ces polluants ont des effets néfastes non seulement sur la santé humaine, mais aussi sur la biodiversité, affectant la flore et la faune locales.

Réduire le trafic automobile permet de préserver les habitats naturels en limitant les perturbations et la dégradation des sols. Les itinéraires dédiés aux vélos et trottinettes sont souvent mieux intégrés dans le paysage naturel, minimisant l'impact sur l'écosystème local.
Une expérience pour tous
La micromobilité permet d'accéder aux zones reculées du parc sans nuire à l'environnement. Parcourir les sentiers et explorer les espaces naturels à l'aide de moyens de transport respectueux des milieux fragiles offre une expérience immersive et respectueuse de la nature.
Imaginez une journée en famille, glissant doucement le long des sentiers ombragés sur des vélos électriques. Découvrez les merveilles de la nature et de la flore luxuriante au Parc Jean-Drapeau, tout en apprenant l'importance de protéger notre environnement. Les arrêts pour admirer un arbre ou un papillon deviennent des moments de partage et d'émerveillement.
La micromobilité offre une manière douce et accessible de se déplacer. Les infrastructures dédiées assurent une expérience sécurisée et agréable. Se déplacer en toute tranquillité, avec le chant des oiseaux, renforce le bien-être et la santé mentale. Des études montrent que l'exposition à des environnements naturels peut réduire le stress, améliorer l'humeur et augmenter le sentiment de bien-être général (Ulrich et al., 1991; Hartig et al., 1991). La micromobilité, en facilitant l'accès à ces espaces naturels, joue un rôle crucial dans la promotion de ces bienfaits.

Équité et accessibilité : une approche inclusive
Il est important de reconnaître que l'accès à la micromobilité n'est pas uniforme pour tous les groupes sociaux. Mon projet de recherche vise à co-créer un système de micromobilité équitable et accessible dans ce milieu naturel. En embrassant cette vision, nous pouvons espérer non seulement des bénéfices environnementaux et de santé publique, mais aussi une transformation sociale où chacun, indépendamment de son genre ou de ses capacités, trouve sa place. Ma recherche au Parc Jean-Drapeau est une aventure pour découvrir comment nous pouvons, ensemble, rendre la micromobilité non seulement une alternative de transport viable, mais aussi une force pour l'équité et le bien-être des visiteurs et des communautés. En intégrant les besoins des groupes sous-représentés, notamment les femmes, les familles, les personnes âgées ou celles à mobilité réduite, nous tisserons un tissu urbain plus équitable et accueillant. Les rires des enfants et les conversations animées des aînés se mêleront aux sons des roues sur les pavés, créant une belle symphonie.
De plus, une intégration de la micromobilité avec les réseaux de transport public – métro, bus, bateau – pourra améliorer l'accessibilité, mais aussi transformer les habitudes de déplacement, réduisant ainsi la dépendance aux voitures individuelles (Oeschger, 2020; Møller et al., 2019).
Une symphonie pour l'avenir
La micromobilité au Parc Jean-Drapeau représente une opportunité unique de promouvoir la durabilité écologique et de protéger la biodiversité locale. En adoptant ces solutions de transport, le parc peut devenir un modèle de conservation urbaine, offrant une expérience enrichissante et respectueuse de l'environnement pour tous ses visiteurs et communautés avoisinantes.
Références
Avila-Palencia, I., Int Panis, L., Dons, E., Gaupp-Berghausen, M., Raser, E., Götschi, T., Gerike, R., Brand, C., de Nazelle, A., Orjuela, J. P., Anaya-Boig, E., Stigell, E., Kahlmeier, S., Iacorossi, F. et Nieuwenhuijsen, M. J. (2018). The effects of transport mode use on self-perceived health, mental health, and social contact measures: A cross-sectional and longitudinal study. Environment International, 120, 199‑206. https://doi.org/10.1016/j.envint.2018.08.002
Bretones, A. et Marquet, O. (2022). Sociopsychological factors associated with the adoption and usage of electric micromobility. A literature review. Transport Policy, 127, 230‑249. https://doi.org/10.1016/j.tranpol.2022.09.008
Bretones, A., Marquet, O., Daher, C., Hidalgo, L., Nieuwenhuijsen, M., Miralles-Guasch, C. et Mueller, N. (2023). Public Health-Led Insights on Electric Micro-mobility Adoption and Use: a Scoping Review. Journal of Urban Health: Bulletin of the New York Academy of Medicine, 100(3), 612‑626. https://doi.org/10.1007/s11524-023-00731-0
Clayton, W. et Musselwhite, C. (2013). Exploring changes to cycle infrastructure to improve the experience of cycling for families. Journal of Transport Geography, 33, 54‑61. https://doi.org/10.1016/j.jtrangeo.2013.09.003
Ghaffar, A., Hyland, M. et Saphores, J.-D. (2023). Meta-analysis of shared micromobility ridership determinants. Transportation Research Part D: Transport and Environment, 121, 103847. https://doi.org/10.1016/j.trd.2023.103847
Hartig, T., Mang, M. et Evans, G. W. (1991). Restorative Effects of Natural Environment Experiences. Environment and Behavior, 23(1), 3‑26. https://doi.org/10.1177/0013916591231001
HEC Montréal Chaire de gestion du secteur de l’énergie. État de l’énergie au Québec 2023. HEC Montréal Chaire de gestion du secteur de l’énergie. https://energie.hec.ca/wp-content/uploads/2023/05/EEQ2023_WEB.pdf 2023.
Milakis, D., Gebhardt, L., Ehebrecht, D. et Lenz, B. (2020). Is micro-mobility sustainable? An overview of implications for accessibility, air pollution, safety, physical activity and subjective wellbeing (p. 180‑189). https://doi.org/10.4337/9781789900477.00030
Møller, T. H., Simlett, J. et Mugnier, E. (2019). Micromobility: Moving cities into a sustainable future - EY Report. https://assets.ey.com/content/dam/ey-sites/ey-com/en_gl/topics/automotive-and-transportation/automotive-transportation-pdfs/ey-micromobility-moving-cities-into-a-sustainable-future.pdf
Mueller, N., Rojas-Rueda, D., Cole-Hunter, T., de Nazelle, A., Dons, E., Gerike, R., Götschi, T., Int Panis, L., Kahlmeier, S. et Nieuwenhuijsen, M. (2015). Health impact assessment of active transportation: A systematic review. Preventive Medicine, 76, 103‑114. https://doi.org/10.1016/j.ypmed.2015.04.010
Oeschger, G., Carroll, P. et Caulfield, B. (2020). Micromobility and public transport integration: The current state of knowledge. Transportation Research Part D: Transport and Environment, 89, 102628. https://doi.org/10.1016/j.trd.2020.102628
Spinney, J. (2006). A Place of Sense: A Kinaesthetic Ethnography of Cyclists on Mont Ventoux. Environment and Planning D: Society and Space, 24(5), 709‑732. https://doi.org/10.1068/d66j
Sun, S. et Ertz, M. (2022). Can shared micromobility programs reduce greenhouse gas emissions: Evidence from urban transportation big data. Sustainable Cities and Society, 85, 104045. https://doi.org/10.1016/j.scs.2022.104045
Şengül, B. et Mostofi, H. (2021). Impacts of E-Micromobility on the Sustainability of Urban Transportation—A Systematic Review. Applied Sciences, 11(13), 5851. https://doi.org/10.3390/app11135851
Ulrich, R. S., Simons, R. F., Losito, B. D., Fiorito, E., Miles, M. A. et Zelson, M. (1991). Stress recovery during exposure to natural and urban environments. Journal of Environmental Psychology, 11(3), 201‑230. https://doi.org/10.1016/S0272-4944(05)80184-7
Au-delà de la biomédecine : les approches écosystémiques de la santé et les efforts de lutte contre la tuberculose dans l’Inuit Nunangat
Pascale Laveault-Allard
le 28 août 2024

(photo personnelle, libre de droits)
La tuberculose demeure une des 10 principales causes de décès mondiales, avec 1,3 million de morts en 2022, selon l’Organisation Mondiale de la Santé. Cette maladie a fait l'objet de nombreuses initiatives de santé publique au cours du dernier siècle. Au Canada, bien que l'incidence soit faible, les communautés de l’Inuit Nunangat sont fortement touchées, avec des taux d'incidence jusqu'à 472 fois supérieurs à ceux de la population non autochtone, atteignant 189 cas pour 100 000 habitants en 2019 (1). Les conditions sociales précaires, telles que l'insécurité alimentaire, le surpeuplement et le manque d'accès aux soins de santé, sont des facteurs déterminants de cette situation (2).
L’histoire de la tuberculose dans l’Inuit Nunangat
L'Inuit Nunangat désigne la terre, l'eau et la glace qui englobe les quatre régions et territoires inuits au Canada : la région désignée des Inuvialuit, le Nunatsiavut, le Nunavik et le Nunavut. L'histoire de la tuberculose dans l'Inuit Nunangat est marquée par des injustices historiques et des pratiques coloniales, apparaissant sur le territoire dès les premiers contacts avec les colons européens.
FIGURE 1. CARTE DE L’INUIT NUNANGAT. SOURCE : WIKIMEDIA CREATIVE COMMONS
De 1940 à 1960, face aux taux alarmants de tuberculose parmi les communautés inuites et des Premières Nations, le gouvernement canadien a mené des campagnes de dépistage massif de la tuberculose, souvent sans consentement et envoyant de force les personnes infectées, principalement des enfants, dans des sanatoriums ou «hôpitaux indiens». Les familles ne savaient pas où leurs proches étaient envoyés ni quand ils reviendraient. Les patients étaient isolés de leur culture et de leur langue pendant des années, recevant souvent des traitements expérimentaux et des interventions chirurgicales non consenties (3). Beaucoup mouraient sans retourner chez eux. Cette période de lutte contre la tuberculose s'est déroulée parallèlement aux politiques d'assimilation, comme les pensionnats et l'identification des Inuit par des numéros, tandis que les équipes de qimmit (chiens de traîneau) étaient tuées par les forces de l'ordre. En 2019, le gouvernement canadien a présenté des excuses officielles pour la piètre gestion de cette épidémie et ses effets néfastes à long terme (4).
Malgré les avancées médicales, la population inuite demeure réticente envers le dépistage, le traitement et la vaccination contre la tuberculose. Les taux élevés de rotation du personnel de santé non autochtone, avec une faible compétence culturelle, entravent la qualité des soins dans les communautés touchées. La lutte contre la tuberculose est également entravée par la méfiance, la mauvaise communication et la stigmatisation (5,6).
Les approches écosystémiques et le double regard, essentiels dans la compréhension de la tuberculose et de ses déterminants
Les pratiques de double regard (two-eyed seeing) s'intègrent dans les approches écosystémiques en santé en combinant les connaissances et les perspectives autochtones avec celles de la science biomédicale. Selon l’organisation Integrative Science, le double regard fait référence à «apprendre à voir d'un œil avec les forces des connaissances autochtones et des modes de savoir, et de l'autre œil avec les forces des connaissances occidentales et des modes de savoir... et apprendre à utiliser ces deux yeux ensemble, dans l'intérêt de tous » (7). Cette intégration permet d'aborder les problèmes de santé de manière holistique, en prenant en compte les dimensions culturelles, sociales, environnementales et économiques. Dans l'Inuit Nunangat, la vision du bien-être est intimement liée à la communauté et au territoire. Les pratiques de guérison et les modes de vie doivent compléter les traitements biomédicaux, offrant des approches de soutien qui sont culturellement acceptables et respectées par les communautés inuites. Toutes ces approches, incluant la vision sanitaire de la santé publique reconnaissent l'importance des déterminants éco-sociaux de la santé, tels que le logement, la sécurité alimentaire, les conditions de vie, le bien-être mental, la langue et la culture, la connexion au territoire et l’accès aux soins, dont plusieurs émergent des injustices systémiques, historiques et coloniales. Une organisation gouvernementale, Inuit Tapiriit Kanatami a d’ailleurs produit un modèle intégré des déterminants inuits de la santé.
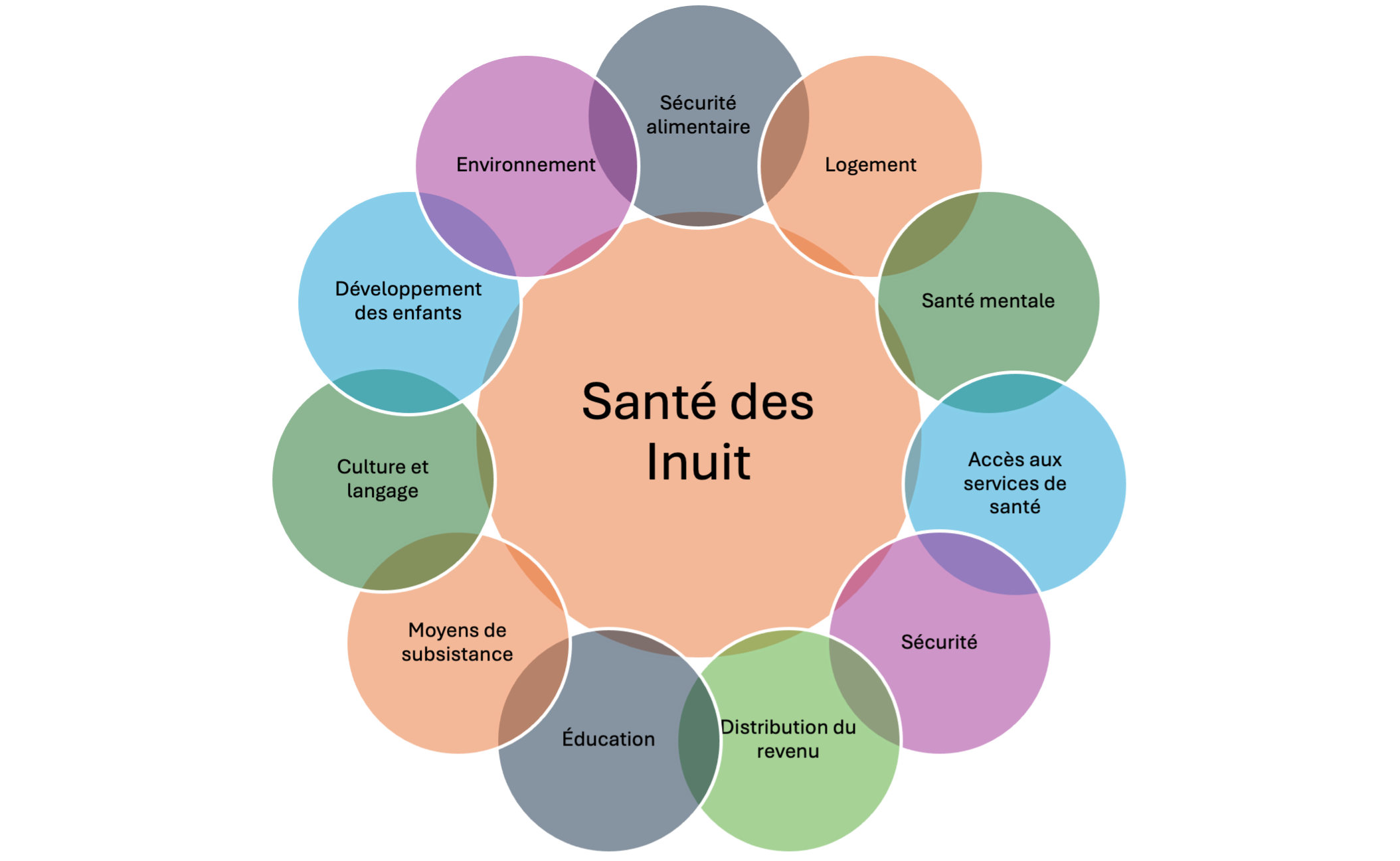
FIGURE 2. DÉTERMINANTS SOCIAUX DE LA SANTÉ INUIT.
ADAPTÉ DE : INUIT TAPIRIIT KANATAMI. (2014) SOCIAL DETERMINANTS OF INUIT HEALTH, OTTAWA.
Les approches de double regard favorisent une collaboration étroite avec les communautés locales, ce qui est essentiel pour une lutte efficace contre la tuberculose (8). Cette collaboration permet une meilleure compréhension mutuelle des causes et des conséquences de la tuberculose, ce qui conduit au développement de politiques publiques culturellement sécuritaires. En valorisant les savoirs autochtones, les interventions de santé gagnent en légitimité et en confiance au sein des communautés, ce qui peut augmenter l'adhésion aux programmes de dépistage et de traitement. De plus, en intégrant les perspectives locales, les communautés Inuit peuvent prendre part aux décisions de santé, renforçant ainsi leur autonomie et leur autodétermination.
Pour conclure, la tuberculose reste un problème complexe dans l'Inuit Nunangat, influencé par des facteurs historiques, sociaux, économiques, environnementaux et sanitaires qui guident les décisions, la répartition des ressources et la confiance des communautés. La biomédecine ne constitue ni le seul défi ni la seule solution face aux inégalités actuelles dans la prévalence de la tuberculose (8,9). Les programmes biomédicaux, souvent teintés de colonialisme et de paternalisme, ne répondent pas aux aspirations d'autonomie et d'autodétermination des Inuit, ni à l'objectif d'élimination de la tuberculose et de ses déterminants éco-sociaux (10). La gestion de la tuberculose dans l'Inuit Nunangat soulève le défi plus large de concilier les approches biomédicales avec les considérations culturelles et historiques propres aux Inuit. Les pratiques de double regard, intégrées naturellement dans les approches écosystémiques en santé, offrent une voie vers des interventions plus complètes et mieux acceptées dans la lutte contre la tuberculose. En combinant les savoirs autochtones et les approches biomédicales, il est possible de développer des solutions de santé respectueuses des valeurs culturelles, adaptées aux besoins locaux et plus efficaces dans la lutte contre la tuberculose. Cela requiert un engagement continu en faveur de l'inclusion, du respect mutuel et de l'intégration des connaissances diversifiées dans toutes les stratégies de santé publique.
Pour en savoir plus:
1. Mounchili A, Perera R, Lee RS, Njoo H, Brooks J. Chapter 1: Epidemiology of tuberculosis in Canada. Can J Respir Crit Care Sleep Med. 24 mars 2022;6(sup1):8‑21.
2. MacDonald N, Hébert PC, Stanbrook MB. Tuberculosis in Nunavut: a century of failure. CMAJ. 19 avr 2011;183(7):741‑741.
3. The dark past and injustices of tuberculosis sanatoria in Canada | APTN InFocus [Internet]. 2017 [cité 9 déc 2023]. Disponible à: https://www.youtube.com/watch?v=rjOCmqMWZKs
4. Trudeau J. Justin Trudeau apologizes on behalf of Canada for mistreatment of Inuit during TB epidemics. [Internet]. 2019 [cité 10 déc 2023]. Disponible à: https://www.youtube.com/watch?v=we4u2LlNfEE
5. Patterson M, Flinn S, Barker K. Addressing tuberculosis among Inuit in Canada. Can Commun Dis Rep Releve Mal Transm Au Can. 1 mars 2018;44(3‑4):82‑5.
6. Møller H. Tuberculosis and Colonialism: Current Tales about Tuberculosis and Colonialism in Nunavut. Int J Indig Health. 2010;6(1):38‑48.
7. Integrative Science. Guiding Principles (Two Eyed Seeing) [Internet]. 2004 [cité 16 mai 2024]. Disponible à: http://www.integrativescience.ca/Principles/TwoEyedSeeing/
8. Martin DH. Two-eyed seeing: a framework for understanding indigenous and non-indigenous approaches to indigenous health research. Can J Nurs Res Rev Can Rech En Sci Infirm. juin 2012;44(2):20‑42.
9. Gray A. The Failure of Western Biomedicine: Treatment of Tuberculosis in the United States. NEXUS Can Stud J Anthropol [Internet]. 1 janv 1996 [cité 6 nov 2023];12(1). Disponible à: https://journals.mcmaster.ca/nexus/article/view/151
10. Long R, Divangahi M, Schwartzman K. Chapter 2: Transmission and pathogenesis of tuberculosis. Can J Respir Crit Care Sleep Med. 24 mars 2022;6(sup1):22‑32.